Since 2014, we have been supporting junior doctors at ASPH with their learning about, and practice of, quality improvement in healthcare. Although the Foundation Year One (F1) doctors are with us for only a short time, we believe there are significant benefits for everyone in providing excellent teaching and support for their QI ideas.
The Be the Change programme was conceived by a group of junior doctors and we are proud to be able to continue to support their professional development and help them to bring about improvements in patient safety and patient experience through small QI projects.
In this blog, we describe how one F1 doctor took his idea for a QI project and created a social movement for improving the lives of patients and staff across our hospitals. It is an amazing story.
The Idea
 Dr Chris Marsh, one of our 2015/16 junior doctors, proposed an idea through the Be the Change programme, having observed the problem of ‘cognitive decline’ among some elderly and long-staying patients on the ASPH wards. Chris was concerned that in some cases, we might be swapping physical illness for mental illness.
Dr Chris Marsh, one of our 2015/16 junior doctors, proposed an idea through the Be the Change programme, having observed the problem of ‘cognitive decline’ among some elderly and long-staying patients on the ASPH wards. Chris was concerned that in some cases, we might be swapping physical illness for mental illness.
Here is how Chris initially described the problem:
“In recent months, working on a ward with a very old average age demographic, I have been struck by the cognitive decline in so many of our long-stay patients for no other reason than the lack of intellectual and social stimulation available to them.
Many of our patients are medically fit for discharge but awaiting social packages of care in the community. Even those fortunate enough to have friends and family visiting – though many do not – will spend by far the majority of their day sat in their beds or chairs staring into space.
Imagine if you or I, fit and healthy as we are, were forced to sit or lie all day in a sterile ward without any social interaction. Now imagine the night time filled with the cries of five strangers, many of whom may be in pain or distress, keeping you from being able to sleep. How would we feel after five, ten, fifty days of that?
I suspect many of us would be in a state of mind qualifying us for a diagnosis of delirium or dementia. Whilst we are very good at diagnosing and treating patients for physical health issues, our system is woefully lacking in taking a holistic caring approach to our patients. Wellbeing can never be achieved by physical health alone.”
Chris’ proposed solution was initially to engage work-experience students or volunteers from local organisations to visit and interact with these patients. However, his initial idea stalled and looked like it wouldn’t be possible due to the requirements for anyone working in a hospital (DBS checks, health clearances, etc).
However, Chris was undeterred and continued to search for a solution to help improve the care provided to patients. Chris found evidence from a recent finance census suggesting that less than half of non-clinical staff felt valued by their clinical colleagues, and arrived at the idea of using non-clinical hospital staff to participate in a volunteer programme.
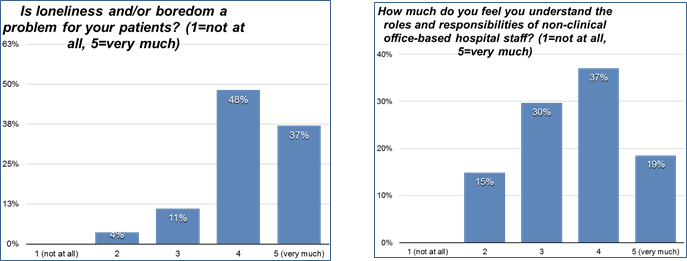
Chris carried out a baseline survey with staff working on our medical wards and the results showed that more than 80% of respondents reported boredom and loneliness as a problem for their patients and close to 50% said that they did not have a clear understanding of the roles of non-clinical staff in the hospital.
The ‘Adopt a Grandparent’ programme was designed and, if successful, would help to connect non-clinical and office-based staff to the core-business of the hospital; as well as improving the well-being of our patients.
Adopt a Grandparent – The Programme
The programme had two aims
1 – To improve social stimulation for longer staying patients and thereby improve clinical outcomes
2 – To break-down barriers between clinical and non-clinical staff within our hospitals
Staff volunteers were recruited and invited to attend an initial workshop, at which the team discussed basic health and safety awareness, communication and what will be required during a ward visit. The volunteers were then allocated to a specific ward and are asked to record their visits in a ward based diary. Regular de-brief meetings were held to collect feedback and share experiences.
The programme now includes a referral system which allows wards to request a visit by emailing the volunteer team to see if someone is available to visit a specific patient.
There is no doubt that this programme is benefitting patients and staff alike and feedback received has been extremely positive. Here’s what one of the volunteers said;
“I have to admit, I was a tiny bit nervous going to the ward for the first time to participate in the initiative. However, I had a lovely chat with an elderly gentleman, and found out a lot about his life. It was lovely to see how he changed from a patient lying in a bed; to the person he truly is, as we engaged in conversation. I left the ward wishing I could have staye d longer and can’t wait to go back again. I think this may become addictive and the highlight of my weeks”
d longer and can’t wait to go back again. I think this may become addictive and the highlight of my weeks”
Adopt a Grandparent was presented by Chris at the Annual DAPS (Doctors Advancing Patient Safety) Global conference in September 2016 and the programme won a DAPS award, it was also shortlisted in two PENN (Patient Experience National Network) Award categories for 2016 and achieved runner up in the ‘Personalisation of Care’ category.
The Future
The Adopt a Grandparent programme continues to run at ASPH, although it is not without its challenges. Engaging and maintaining contact with the staff volunteers is a significant task and this shouldn’t be underestimated. The team have started to recruit volunteers via the monthly corporate induction programme for new staff and regular internal communication is maintained to encourage more staff to participate.
We are really pleased that this simple idea for a QI project has (with no additional costs) been able to harness our staff’s natural enthusiasm and deliver improvements for patients.
Lessons Learned / Top Tips
- Don’t give up on an idea, even if your initial plans don’t seem possible
- If something is the right thing to do for patient wellbeing, then there will be support
- Ask for help – Chris’ idea was pretty big and he was not in a position to influence all the people that needed to be involved, he enlisted the help of the ‘Be the Change’ team and together we made it possible
- Share your ideas and good practice – Adopt a Grandparent has generated a lot of interest from other Trusts and we have been more than happy to share our idea
If you want to find out more about the programme you can contact the team via AdoptaGrandparent@asph.nhs.uk and just let us know your thoughts in the comments section below.
Thanks,
Sally – @Sally2PT
